Asociación entre tiroiditis linfocítica crónica y carcinoma papilar de tiroides: Revisión sistemática y metaanálisis de estudios en especímenes quirúrgicos
DOI:
https://doi.org/10.30944/20117582.2228Palabras clave:
carcinoma papilar de tiroides, tiroiditis linfocítica crónica, especímenes quirúrgicos, estudio retrospectivo, revisión sistemática, metaanálisisResumen
Introducción. Existen resultados inconsistentes con relación al planteamiento de la hipótesis que sugiere una mayor probabilidad de documentar un carcinoma papilar de tiroides en especímenes quirúrgicos con cambios compatibles con tiroiditis linfocítica crónica. En los metaanálisis se han incluido estudios no comparables metodológicamente y no se proponen claras fuentes de sesgo, justificación para la realización del presente estudio.
Métodos. Se realizó una búsqueda bibliográfica en PubMed y Embase. Fueron obtenidos estudios retrospectivos donde se comparaba la prevalencia de carcinoma papilar de tiroides en especímenes con y sin cambios por tiroiditis linfocítica crónica. La evidencia recolectada fue sintetizada estadísticamente.
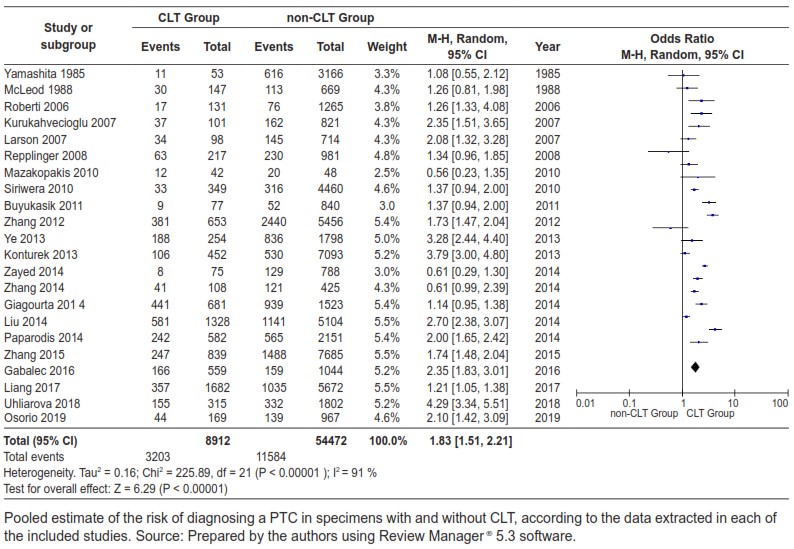
Resultados. Un total de 22 artículos fueron incluidos. La población estuvo conformada por 63.548 especímenes. El OR combinado fue 1,81 (IC95%: 1,51-2,21). Hubo heterogeneidad en la distribución de las razones de oportunidad entre los estudios (I2 = 91 %; p>0,00001). La forma del gráfico en embudo de los estudios incluidos en el análisis parece estar simétrica, lo que indica la ausencia del sesgo atribuible a los estudios pequeños.
Conclusiones. La literatura actual sugiere que existe un mayor riesgo de documentar un carcinoma papilar de tiroides en especímenes quirúrgicos en los que se observan cambios compatibles con tiroiditis linfocítica crónica; sin embargo, existen fuentes de sesgo que no será posible controlar en estudios retrospectivos, por lo que recomendamos estudiar la hipótesis que sugiere una mayor probabilidad de diagnosticar un carcinoma papilar de tiroides en especímenes con cambios compatibles con tiroiditis linfocítica crónica mediante metodologías prospectivas.
Descargas
Referencias bibliográficas
Rosai J, Albores Saavedra J, Asioli S, Baloch ZW, Bogdanova T, Chen H, et al. Papillary Thyroid Carcinoma. In: WHO Classification of Tumours of Endocrine Organs 4th edition. (Lloyd RV, Osamura RY, Klöppel G, Rosai J. eds.). IARC: Lyon; 2017. pp. 81-92.
Siegel R, Naishadham D, Jemal A. Cancer statistics 2013. CA Cancer J Clin. 2013;63:11-30. https://doi.org/10.3322/caac.21166
Soares P, Celestino R, Gaspar da Rocha A, Sobrinho-Simões M. Papillary thyroid microcarcinoma: ¿How to diagnose and manage this epidemic? Int J Surg Pathol. 2014;22:113-9. https://doi.org/10.1177/1066896913517394
Siegel RL, Miller KD, Fuch HE, Jemal A. Cancer statistics 2022. CA Cancer J Clin. 2022;72:7-33. https://doi.org/10.3322/caac.21708
Bongiovanni M, Giovanella L, Romanelli F, Trimboli P. Cytological diagnosis associated with noninvasive follicular thyroid neoplasms with papillary-like nuclear features according to the Bethesda system for reporting thyroid cytopathology: A systematic review and meta-analysis. Thyroid. 2019;29:222-8. https://doi.org/10.1089/thy.2018.0394
Caturegli P, De Remigis A, Rose N. Hashimoto thyroiditis: clinical and diagnostic criteria. Autoimmun Rev. 2014;13:391-7. https://doi.org/10.1016/j.autrev.2014.01.007
Huber G, Staub JJ, Meier C, Mitrache C, Guglielmetti M, Huber P, et al. Prospective study of the espontaneous course of subclinical hypothyroidism: prognostic value of thyrotropin, thyroid reserve, and thyroid antibodies. J Clin Endocrinol Metab. 2002;87:3221-6. https://doi.org/10.1210/jcem.87.7.8678
Zaletel K, Gaberscek S. Hashimoto´s thyroiditis: From genes to the disease. Curr Genomics. 2011;12:576-88. https://doi.org/10.2174/138920211798120763
Nosé V. Hashimoto Thyroiditis. In: Diagnostic Pathology: Endocrine. 2nd edition (Nosé V, Cipriani N, Fisch A, eds). Canadá: Elsevier Health Sciences; 2018; pp 53-60.
Lindsay S, Dailey ME, Friedlander J, Yee G, Soley MG. Chronic thyroiditis: a clinical and pathologic study of 354 patients. J Clin Endocrinol Metab. 1952;12:1578- 1600. https://doi.org/10.1210/jcem-12-12-1578
Dailey M, Lindsay S, Skahen R. Relation of thyroid neoplasms to Hashimoto disease of the thyroid gland. AMA Arch Surg. 1955;70:291-7. https://doi.org/10.1001/archsurg.1955.01270080137023
Holm L, Blomgren H, Löwhagen T. Cancer risk in patients with chronic lymphocytic thyroiditis. N Engl J Med. 1985;312:601-4. https://doi.org/10.1056/NEJM198503073121001
Anil C, Goksel S, Gursoy A. Hashimoto’s thyroiditis is not associated with increased risk of thyroid cancer in patients with thyroid nodules: a single-center prospective study. Thyroid. 2010;20:601-6. https://doi.org/10.1089/thy.2009.0450
Le K, Hershman J. Hashimoto´s thyroiditis does not predispose patients to differentiated thyroid cancer. Clin Thyroidology. 2014;26:227-9. https://doi.org/10.1089/ct.2014;26.227-229
Singh B, Shaha AR, Trivedi H, Carew JF, Poluri A, Shah JP. Coexistent Hashimoto’s thyroiditis with papillary thyroid carcinoma: impact on presentation, management, and outcome. Surgery. 1999;126:1070-7. https://doi.org/10.1067/msy.2099.101431
Lee JH, Kim Y, Choi JW, Kim YS. The association between papillary thyroid carcinoma and histologically proven Hashimoto’s thyroiditis: a meta-analysis. Eur J Endocrinol. 2013;168:343-9. https://doi.org/10.1530/EJE-12-0903
Lai X, Xia Y, Zhang B, Li J, Jiang Y. A meta-analysis of Hashimoto’s thyroiditis and papillary thyroid carcinoma risk. Oncotarget. 2017;8:62414-24. https://doi.org/10.18632/oncotarget.18620
Resende de Paiva C, Grønhøj C, Feldt-Rasmussen U, von Buchwald C. Association between Hashimoto’s thyroiditis and thyroid cancer in 64,628 patients. Front Oncol. 2017;7:53. https://doi.org/10.3389/fonc.2017.00053
Jankovic B, Le K, Hershman J. Hashimoto’s thyroiditis and papillary thyroid carcinoma: is there a correlation? J Clin Endocrinol Metab. 2013;98:474-82. https://doi.org/10.1210/jc.2012-2978
Holm L, Blomgren H, Löwhagen T. Cancer risks in patients with chronic lymphocytic thyroiditis. N Engl J Med. 1985;312:601-4. https://doi.org/10.1056/NEJM19850307312100
Gul K, Dirikoc A, Kiyak G, Ersoy P, Ugras N, Ersoy R, et al. The association between thyroid carcinoma and Hashimoto’s thyroiditis: the ultrasonographic and histopathologic characteristics of malignant nodules. Thyroid. 2010;20:873-8. https://doi.org/10.1089/thy.2009.0118
Alcântara-Jones D, Alcântara-Nunes T, Rocha B, Oliveira R, Santa A, Alcântara F, et al. Is there any association between Hashimoto’s thyroiditis and thyroid cancer? A retrospective data analysis. Radiol Bras. 2015;48:148-53. https://doi.org/10.1590/0100-3984.2014.0072
Matesa-Anić D, Matesa N, Dabelić N, Kusić Z. Coexistence of papillary carcinoma and Hashimoto’s thyroiditis. Acta Clin Croat. 2009;48:9-12.
Gómez J, Gómez N, Sahun M, Soler J. Prevalence and significance of lymphocyte infiltration in papillary carcinoma of the thyroid gland. Ann Med Int. 1997;14:403-5.
Asanuma K, Sugenoya A, Kasuga Y, Itoh N, Kobayashi S, Amano J. The relationship between multiple intrathyroidal involvement in papillary thyroid carcinoma and chronic non-specific thyroiditis. Cancer Lett. 1998;122:177-80. https://doi.org/10.1016/s0304-3835(97)00398-4
Loh K, Greenspan F, Dong F, Miller T, Yeo P. Influence of lymphocytic thyroiditis on the prognostic outcome of patients with papillary thyroid carcinoma. J Clin Endocrinol Metab. 1999;84:458-63. https://doi.org/10.1210/jcem.84.2.5443
Kebebew E, Treseler P, Ituarte P, Clark O. Coexisting chronic lymphocytic thyroiditis and papillary thyroid cancer revisited. World J Surg. 2001;25:632-7. https://doi.org/10.1007/s002680020165
Tamimi D. The association between chronic lymphocytic thyroiditis and thyroid tumors. Int J Surg Pathol. 2002;10:141-6. https://doi.org/10.1177/106689690201000207
Cipolla C, Sandonato L, Graceffa G, Fricano S, Torcivia A, Vieni S, et al. Hashimoto thyroiditis coexistent with papillary thyroid carcinoma. Am Surg. 2005;71:874-8. https://doi.org/10.1177/000313480507101018
Del Rio P, Cataldo S, Sommaruga L, Kim Y. The association between papillary carcinoma and chronic lymphocytic thyroiditis: does it modify the prognosis of cancer? Minerva Endocrinologica. 2008;33:1-5.
Muzza M, Degl’Innocenti D, Colombo C, Perrino M, Elena R, Rossi S, et al. The tight relationship between papillary thyroid cancer, autoimmunity and inflammation: clinical and molecular studies. Clin Endocrinol (Oxf). 2010;72:702-8. https://doi.org/10.1111/j.1365-2265.2009.03699.x
Huang B, Hseuh C, Chao T, Lin K, Lin J. Well-differentiated thyroid carcinoma with concomitant Hashimoto’s thyroiditis present with less aggressive clinical stage and low recurrence. Endocr Pathol. 2011;22:144-9. https://doi.org/10.1007/s12022-011-9164-9
Yoon Y, Kim H, Lee J, Kim J, Koo B. The clinicopathologic differences in papillary thyroid carcinoma with or without co-existing chronic lymphocytic thyroiditis. Eur Arch Otorhinolaryngoly. 2012;269:1013-7. https://doi.org/10.1007/s00405-011-1732-6
Liberati A, Altman D, Tetzlaff J, Mulrow C, Gøtzsche P, Ioannidis J, et al. The PRISMA statement for reporting systematic reviews and meta-analyses of studies that evaluate health care interventions: explanation and elaboration. BMJ. 2009;339:b2700. https://doi.org/10.1136/bmj.b2700
Moher D, Liberati A, Tetzlaff J, Altman D, The PRISMA Group (2009). Preferred reporting items for systematic reviews and meta-analyses: The PRISMA statement. PLoS Med. 2009;6:332-6. https://doi.org/10.1136/bmj.b2535
Dailey M, Lindsay S, Skahen R. Relation of thyroid neoplasms to Hashimoto disease of the thyroid gland. AMA Arch Surg 1955;70:291-7. https://doi.org/10.1001/archsurg.1955.01270080137023
Okayasu I, Fujiwara M, Hara Y, Tanka Y, Rose N. Association of chronic lymphocytic thyroiditis and thyroid papillary carcinoma. A study of surgical cases among Japanese, and white and African Americans. Cancer. 1995;76:2312-8. https://doi.org/10.1002/1097-0142(19951201)76:1 13.0.co;2-h
Bradly DP, Reddy V, Prinz RA, Gattuso P. Incidental papillary carcinoma in patients treated surgically for benign thyroid diseases. Surgery 2009;146:1099-104. https://doi.org/10.1016/j.surg.2009.09.025
Consorti F, Loponte M, Milazzo F, Potasso L, Antonasi A. Risk of malignancy from thyroid nodular disease as an element of clinical management of patients with Hashimoto’s thyroiditis. Eur Surg Res 2010;45:333-7. https://doi.org/10.1159/000320954
Ahn D, Heo S, Park J, Kim J, Sohn J, Park J, et al. Clinical relationship between Hashimoto’s thyroiditis and papillary thyroid cancer. Acta Oncol 2011;50:1228-34. https://doi.org/10.3109/0284186X.2011.602109
Kim K, Park Y, Kim E, Park S, Park D, Ahn S, et al. Elevated risk of papillary thyroid cancer in Korean patients with Hashimoto’s thyroiditis. Head Neck. 2011;33:691- 5. https://doi.org/10.1002/hed.21518
Lun Y, Wu X, Xia Q, Han Y, Zhang X, Liu Z, et al. Hashimoto’s thyroiditis as a risk factor of papillary thyroid cancer may improve cancer prognosis. Otolaryngol Head Neck Surg. 2013;148:396-402. https://doi.org/10.1177/0194599812472426
Kutluturk K, Unal B, Cetin S. Coexistence of Hashimoto’s thyroiditis with papillary thyroid carcinoma: a single center experience. J Turgut Ozal Med Cent. 2017;24:190-2. https://doi.org/10.5455/jtomc.2017.03.34
Lee I, Hsieh A, Lee T, Lee T, Chien Y. The association of thyrotropin and autoimmune thyroid disease in developing papillary thyroid cancer. Int J Endocrinol. 2017;2017:5940367. https://doi.org/10.1155/2017/5940367
Nawarathna N, Ratnayake P, Hewage S, Senevirathne J, Gunatilake S, Kariyawasam N, et al. Association between nonspecific chronic lymphocytic thyroiditis and differentiated epithelial thyroid carcinoma: Clinicopathological analysis of patients who underwent thyroidectomy in a tertiary care center in Sri Lanka. World J Endoc Surg. 2018;10:119-26. https://doi.org/10.5005/jp-journals-10002-1230
Jackson D, Handelsman R, Farrá J, Lew J. Increased incidental thyroid cancer in patients with subclinical chronic lymphocytic thyroiditis. J Surg Res. 2020;245:115-8. https://doi.org/10.1016/j.jss.2019.07.025
Peterson C, Shidler F. Lymphocytic thyroiditis in 757 thyroid operations. Am J Surg. 1957;94:223-31. https://doi.org/10.1016/0002-9610(57)90649-9
Shands W. Carcinoma of the thyroid in association with struma lymphomatosa (Hashimoto’s disease). Ann Surg. 1960;151:675-82. https://doi.org/10.1097/00000658-196005000-00008
Campos L, Picado S, Guimarães A, Ribeiro D, Dedivitis R. Thyroid papillary carcinoma associated to Hashimoto’s thyroiditis. Braz J Otorhinolaryngol. 2012;78:77-80. https://doi.org/10.5935/1808-8694.20120037
Yamashita H, Nakayama I, Noguchi S, Murakami N, Moriuchi A, Yokoyama S, et al. Thyroid carcinoma in benign thyroid diseases. An analysis from minute carcinoma. Acta Pathol Jpn. 1985;35:781-8. https://doi.org/10.1111/j.1440-1827.1985.tb00620.x
McLeod M, East M, Burney R, Harness J, Thompson N. Hashimoto’s thyroiditis revisited: the association with thyroid cancer remains obscure. World J Surg. 1988;12:509-6. https://doi.org/10.1007/BF01655435
Roberti A, Sobrinho J, Porto O, Rapoport A. Concomitância da tireoidite de Hashimoto e o carcinoma diferenciado da tireóide. Rev Col Bras Cir. 2006;33:345-9. https://doi.org/10.1590/S0100-69912006000600003
Kurukahvecioglu O, Taneri F, Yüksel O, Aydin A, Tezel E, Onuk E. Total thyroidectomy for the treatment of Hashimoto’s thyroiditis coexisting with papillary thyroid carcinoma. Adv Ther. 2007;24:510-6. https://doi.org/10.1007/BF02848773
Larson S, Jackson L, Riall T, Uchida T, Thomas R, Qiu S, et al. Increased incidence of well-differentiated thyroid cancer associated with Hashimoto thyroiditis and the role of the PI3k/Akt pathway. J Am Coll Surg. 2007;204:764-75. https://doi.org/10.1016/j.jamcollsurg.2006.12.037
Repplinger D, Bargren A, Zhang YW, Adler JT, Haymart M, Chen H. Is Hashimoto’s thyroiditis a risk factor for papillary thyroid cancer? J Surg Res. 2008;150:49-52. https://doi.org/10.1016/j.jss.2007.09.020
Mazokopakis E, Tzortzinis A, Dalieraki-Ott E, Tsartsalis A, Syros P, Karefilakis C, et al. Coexistence of Hashimoto’s thyroiditis with papillary thyroid carcinoma. A retrospective study. Hormones (Athens). 2010;9:312-7. https://doi.org/10.14310/horm.2002.1282
Siriweera E, Ratnatunga N. Profile of Hashimoto’s thyroiditis in Sri Lankans: Is there an increased risk of ancillary pathologies in Hashimoto’s thyroiditis? J Thyroid Res. 2010;2010:124264. https://doi.org/10.4061/2010/124264
Buyukasik O, Hasdemir A, Yalcin E, Celep B, Sengul S, Yandakci K, et al. The association between thyroid malignancy and chronic lymphocytic thyroiditis: should it alter the surgical approach? Endokrynol Pol. 2011; 4:303-8.
Zhang L, Li H, Ji Q, Zhu Y,Wang Z, Wang Y,et al. The clinical features of papillary thyroid cancer in Hashimoto’s thyroiditis patients from an area with a high prevalence of Hashimoto’s disease. BMC Cancer. 2012;12:610. https://doi.org/10.1186/1471-2407-12-610
Konturek A, Barczyński M, Wierzchowski W, Stopa M, Nowak W. Coexistence of papillary thyroid cancer with Hashimoto thyroiditis. Langenbecks Arch Surg. 2013;398:389-94. https://doi.org/10.1007/s00423-012-1021-x
Ye Z, Gu D, Hu H, Zhou Y, Hu X, Zhang X. Hashimoto’s thyroiditis, microcalcification and raised thyrotropin levels within normal range are associated with thyroid cancer. World J Surg Oncol. 2013;11:56. https://doi.org/10.1186/1477-7819-11-56
Giagourta I, Evangelopoulou C, Papaioannou G, Kassi G, Zapanti E, Prokopiou M, et al. Autoimmune thyroiditis in benign and malignant thyroid nodules: 16-year results. Head Neck. 2014;36:531-5. https://doi.org/10.1002/hed.23331
Liu X, Zhu L, Cui D, Wang Z, Chen H, Duan Y, et al. Coexistence of histologically confirmed Hashimoto’s thyroiditis with different stages of papillary thyroid carcinoma in a consecutive chinese cohort. Int J Endocrinol. 2014;2014:769294. https://doi.org/10.1155/2014/769294
Paparodis R, Imam S, Todorova-Koteva K, Staii A, Jaume J. Hashimoto’s thyroiditis pathology and risk for thyroid cancer. Thyroid. 2014;24:1107-14. https://doi.org/10.1089/thy.2013.0588
Zayed A, Ali M, Jaber O, Suleiman M, Ashhab A, Al Shweiat W, et al. Is Hashimoto’s thyroiditis a risk factor for medullary thyroid carcinoma? Our experience and a literature review. Endocrine. 2015;48:629-36. https://doi.org/10.1007/s12020-014-0363-2
Zhang Y, Ma X, Deng F, Liu Z, Wei H, Wang X, et al. The effect of chronic lymphocytic thyroiditis on patients with thyroid cancer. World J Surg Oncol. 2014;12:277. https://doi.org/10.1186/1477-7819-12-277
Zhang Y, Dai J, Wu T, Yang N, Yin Z. The study of the coexistence of Hashimoto’s thyroiditis with papillary thyroid carcinoma. J Cancer Res Clin Oncol. 2014;140:1021-6. https://doi.org/10.1007/s00432-014-1629-z
Gabalec F, Srbova L, Nova M, Hovorkova E, Hornychova H, Jakubikova I, et al. Impact of Hashimoto’s thyroiditis, TSH levels, and anti-thyroid antibody positivity on differentiated thyroid carcinoma incidence. Endokrynol Pol. 2016;67:48-53. https://doi.org/10.5603/EP.a2016.0022
Liang J, Zeng W, Fang F, Yu T, Zhao Y, Fan X, et al. Clinical analysis of Hashimoto thyroiditis coexistent with papillary thyroid cancer in 1392 patients. Acta Otorhinolaryngol Ital. 2017;37:393-400. https://doi.org/10.14639/0392-100X-1709
Uhliarova B, Hajtman A. Hashimoto’s thyroiditis - an independent risk factor for papillary carcinoma. Braz J Otorhinolaryngol. 2018;84:729-35. https://doi.org/10.1016/j.bjorl.2017.08.012
Osorio C, Ibarra S, Arrieta J, Sarmiento M, Barrios D, Sierra L, et al. Association between chronic lymphocytic thyroiditis and papillary thyroid carcinoma: A retrospective study in surgical specimens. Rev Esp Patol. 2020;53:149-57. https://doi.org/10.1016/j.patol.2019.07.004
Descargas
Publicado
Cómo citar
Número
Sección
Licencia
Derechos de autor 2022 Revista Colombiana de Cirugía

Esta obra está bajo una licencia internacional Creative Commons Atribución-NoComercial-SinDerivadas 4.0.
Todos los textos incluidos en la Revista Colombiana de Cirugía están protegidos por derechos de autor. Las opiniones expresadas en los artículos firmados son las de los autores y no coinciden necesariamente con las de los directores o los editores de la Revista Colombiana de Cirugía. Las sugerencias diagnósticas o terapéuticas como elección de productos, dosificación y métodos de empleo corresponden a la experiencia y al criterio de los autores.

















.jpg)


