Infección temprana de la malla quirúrgica en herniorrafia incisional. Incidencia, factores de riesgo y desenlaces en más de 60.000 pacientes
DOI:
https://doi.org/10.30944/20117582.1119Palabras clave:
hernia incisional, herniorrafia, incidencia, factores de riesgo, complicaciones postoperatoriasResumen
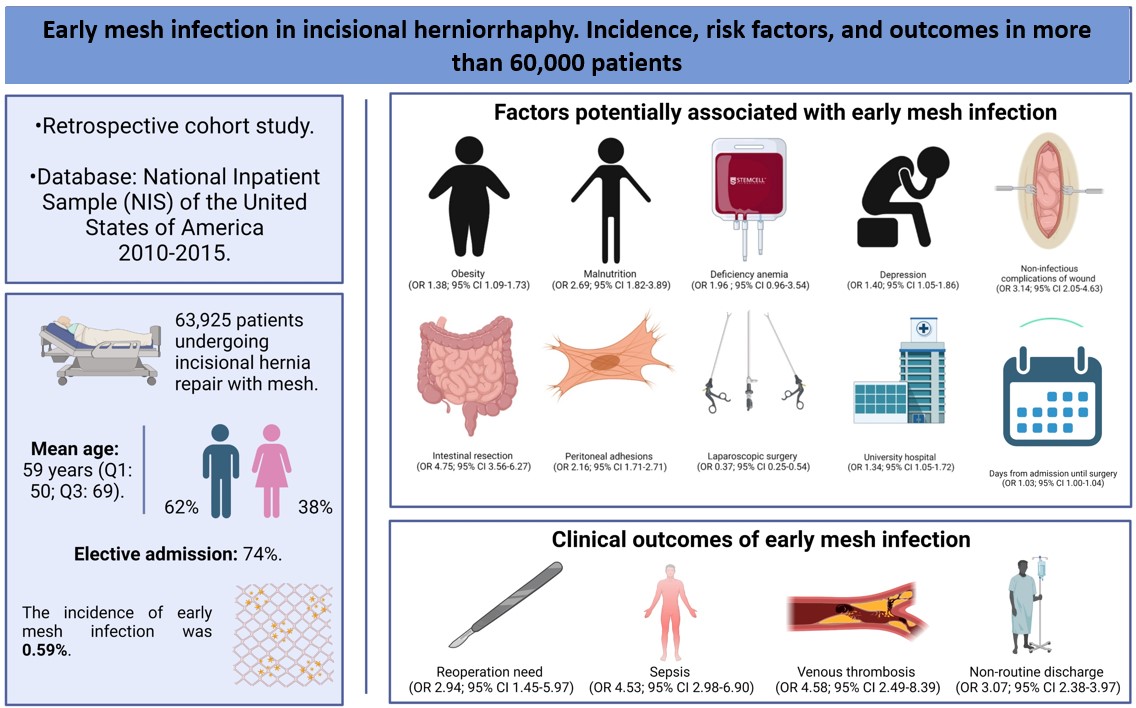
Introducción. La infección de la malla en cirugía de reparación de hernias de pared abdominal es un desenlace pobre, asociado a un incremento en el riesgo de complicaciones. El objetivo del presente estudio fue analizar la incidencia, los factores asociados y desenlaces en pacientes llevados a herniorrafia incisional con malla con posterior diagnóstico de infección temprana.
Métodos. Estudio de cohorte retrospectiva. Se utilizaron los datos de egresos hospitalarios de la National Inpatient Sample (NIS) de los Estados Unidos de América para identificar a todos los pacientes adultos llevados a herniorrafia incisional durante los años 2010 a 2015. Se utilizaron modelos de regresión logística bivariada y multivariada para evaluar los factores de riesgo en infección temprana de la malla, y finalmente, modelos de regresión logística y lineal, según el tipo de variable dependiente, de tipo stepwise forward para evaluar la asociación entre el diagnóstico de infección de malla y los desenlaces adversos.
Resultados. En total se incluyeron 63.925 pacientes. La incidencia de infección temprana de la malla fue de 0,59 %, encontrando como factores asociados: comorbilidades (obesidad, desnutrición proteico calórica, anemia carencial y depresión), factores clínico-quirúrgicos (adherencias peritoneales, resección intestinal, cirugía laparoscópica y complicaciones no infecciosas de la herida) y administrativos o asistenciales.
Conclusiones. La infección temprana, aunque infrecuente, se asocia con un aumento significativo en el riesgo de complicaciones. La optimización prequirúrgica con base en los factores de riesgo para este desenlace nefasto es un elemento clave para la reducción de la incidencia y mitigación del impacto de la infección en los pacientes con herniorrafía incisional con malla.
Descargas
Referencias bibliográficas
Plymale MA, Davenport DL, Walsh-Blackmore S, Hess J, Griffiths WS, Plymale MC, et al. Costs and complications associated with infected mesh for ventral hernia repair. Surg Infect. 2020;21:344-9. https://doi.org/10.1089/sur.2019.183
Hawn MT, Gray SH, Snyder CW, Graham LA, Finan KR, Vick CC. Predictors of mesh explantation after incisional hernia repair. Am J Surg. 2011;202:28-33. https://doi.org/10.1016/j.amjsurg.2010.10.011
Tastaldi L, Petro CC, Krpata DM, Alkhatib H, Fafaj A, Tu C, et al. History of surgical site infection increases the odds for a new infection after open incisional hernia repair. Surgery. 2019;166:88-93. https://doi.org/10.1016/j.surg.2019.01.032
Brown RH, Subramanian A, Hwang CS, Chang S, Awad SS. Comparison of infectious complications with synthetic mesh in ventral hernia repair. Am J Surg. 2013;205:182-7. https://doi.org/10.1016/j.amjsurg.2012.02.023
Sanchez VM, Abi-Haidar YE, Itani KMF. Mesh infection in ventral incisional hernia repair: incidence, contributing factors, and treatment. Surg Infect. 2011;12:205-10. https://doi.org/10.1089/sur.2011.033
Dipp Ramos R, O’Brien WJ, Gupta K, Itani KMF. Incidence and risk factors for long-term mesh explantation due to infection in more than 100,000 hernia operation patients. J Am Coll Surg. 2021;232:872-880.e2. https://doi.org/10.1016/j.jamcollsurg.2020.12.064
Bueno-Lledó J, Torregrosa-Gallud A, Sala-Hernandez A, Carbonell-Tatay F, Pastor PG, Diana SB, et al. Predictors of mesh infection and explantation after abdominal wall hernia repair. Am J Surg. 2017;213:50-7. https://doi.org/10.1016/j.amjsurg.2016.03.007
Pérez-Köhler B, Bayon Y, Bellón JM. Mesh infection and hernia repair: a review. Surg Infect. 2016;17:124-37. https://doi.org/10.1089/sur.2015.078
Falagas ME, Kasiakou SK. Mesh-related infections after hernia repair surgery. Clin Microbiol Infect. 2005;11:3- 8. https://doi.org/10.1111/j.1469-0691.2004.01014.x
Carlson MA, Frantzides CT, Shostrom VK, Laguna LE. Minimally invasive ventral herniorrhaphy: an analysis of 6,266 published cases. Hernia. 2008;12:9-22. https://doi.org/10.1007/s10029-007-0286-4
Narkhede R, Shah NM, Dalal PR, Mangukia C, Dholaria S. Postoperative mesh infection—still a concern in laparoscopic era. Indian J Surg. 2015;77:322-6. https://doi.org/10.1007/s12262-015-1304-x
Bamgbade OA, Rutter TW, Nafiu OO, Dorje P. Postoperative complications in obese and nonobese patients. World J Surg. 2007;31:556-61. https://doi.org/10.1007/s00268-006-0305-0
Tjeertes EEKM, Hoeks SSE, Beks SSBJC, Valentijn TTM, Hoofwijk AAGM, Stolker RJRJ. Obesity – a risk factor for postoperative complications in general surgery? BMC Anesthesiol. 2015;15:112. https://doi.org/10.1186/s12871-015-0096-7
Castoldi A, Naffah de Souza C, Câmara NOS, Moraes-Vieira PM. The macrophage switch in obesity development. Front Immunol. 2016;6:637. https://doi.org/10.3389/fimmu.2015.00637
Pence BD, Woods JA. Exercise, obesity, and cutaneous wound healing: evidence from rodent and human studies. Adv Wound Care (New Rochelle). 2014;3:71-9. https://doi.org/10.1089/wound.2012.0377
Pierpont YN, Dinh TP, Salas RE, Johnson EL, Wright TG, Robson MC, et al. Obesity and surgical wound healing: a current review. ISRN Obes. 2014;638936. https://doi.org/10.1155/2014/638936
Tsantes AG, Papadopoulos DV, Lytras T, Tsantes AE, Mavrogenis AF, Korompilias AV, et al. Association of malnutrition with periprosthetic joint and surgical site infections after total joint arthroplasty: a systematic review and meta-analysis. J Hosp Infect. 2019;103:69- 77. https://doi.org/10.1016/j.jhin.2019.04.020
Tsantes AG, Papadopoulos DV, Lytras T, Tsantes AE, Mavrogenis AF, Koulouvaris P, et al. Association of malnutrition with surgical site infection following spinal surgery: systematic review and meta-analysis. J Hosp Infect. 2020;104:111-9. https://doi.org/10.1016/j.jhin.2019.09.015
de Luis DA, Culebras JM, Aller R, Eiros-Bouza JM. Surgical infection and malnutrition. Nutr Hosp. 2014;30:509-13.
Stechmiller JK. Understanding the role of nutrition and wound healing. Nutr Clin Pract. 2010;25:61-8. https://doi.org/10.1177/0884533609358997
Bourke CD, Berkley JA, Prendergast AJ. Immune dysfunction as a cause and consequence of malnutrition. Trends Immunol. 2016;37:386-98. https://doi.org/10.1016/j.it.2016.04.003
Grimble RF. Malnutrition and the immune response. 2. Impact of nutrients on cytokine biology in infection. Trans R Soc Trop Med Hyg. 1994;88:615-9. https://doi.org/10.1016/0035-9203(94)90195-3
Schaible UE, Kaufmann SHE. Malnutrition and infection: complex mechanisms and global impacts. PLoS Med. 2007;4:e115. https://doi.org/10.1371/journal.pmed.0040115
Weber WP, Zwahlen M, Reck S, Misteli H, Rosenthal R, Buser AS, et al. The association of preoperative anemia and perioperative allogeneic blood transfusion with the risk of surgical site infection. Transfusion. 2009;49:1964-70. https://doi.org/10.1111/j.1537-2995.2009.02204.x
Malone DL, Genuit T, Tracy JK, Gannon C, Napolitano LM. Surgical site infections: reanalysis of risk factors. J Surg Res. 2002;103:89-95. https://doi.org/10.1006/jsre.2001.6343
White MC, Longstaff L, Lai PS. Effect of preoperative anaemia on postoperative complications in low resource settings. World J Surg. 2017;41:644-9. https://doi.org/10.1007/s00268-016-3785-6
Howard DPJ, Datta G, Cunnick G, Gatzen C, Huang A. Surgical site infection rate is lower in laparoscopic than open colorectal surgery. Colorectal Dis. 2010;12:423-7. https://doi.org/10.1111/j.1463-1318.2009.01817.x
Suh YJ, Jeong S-Y, Park KJ, Park J-G, Kang S-B, Kim D-W, et al. Comparison of surgical-site infection between open and laparoscopic appendectomy. J Korean Surg Soc. 2012;82:35-9. https://doi.org/10.4174/jkss.2012.82.1.35
Varela JE, Wilson SE, Nguyen NT. Laparoscopic surgery significantly reduces surgical-site infections compared with open surgery. Surg Endosc. 2010;24:270-6. https://doi.org/10.1007/s00464-009-0569-1
Aimaq R, Akopian G, Kaufman HS. Surgical site infection rates in laparoscopic versus open colorectal surgery. Am Surg. 2011;77:1290-4. https://doi.org/10.1177/000313481107701003
Shabanzadeh DM, Sørensen LT. Laparoscopic surgery compared with open surgery decreases surgical site infection in obese patients: a systematic review and meta-analysis. Ann Surg. 2012;256:934-45. https://doi.org/10.1097/SLA.0b013e318269a46b
Ejaz A, Spolverato G, Kim Y, Wolfgang CL, Hirose K, Weiss M, et al. The impact of resident involvement on surgical outcomes among patients undergoing hepatic and pancreatic resections. Surgery. 2015;158:323-30. https://doi.org/10.1016/j.surg.2015.01.027
Kiran RP, Ahmed Ali U, Coffey JC, Vogel JD, Pokala N, Fazio VW. Impact of resident participation in surgical operations on postoperative outcomes: National Surgical Quality Improvement Program. Ann Surg. 2012;256:469-75. https://doi.org/10.1097/SLA.0b013e318265812a
Deng H, Chan A, Ammanuel S, Chan A, Oh T, Skrehot H, et al. Risk factors for deep surgical site infection following thoracolumbar spinal surgery. J Neurosurg Spine. 2019;32:292-301. https://doi.org/10.3171/2019.8.SPINE19479
Olsen MA, Nepple JJ, Riew KD, Lenke LG, Bridwell KH, Mayfield J, et al. Risk factors for surgical site infection following orthopaedic spinal operations. J Bone Joint Surg Am. 2008;90:62-9. https://doi.org/10.2106/JBJS.F.01515
Cheng H, Chen BP-H, Soleas IM, Ferko NC, Cameron CG, Hinoul P. Prolonged operative duration increases risk of surgical site infections: a systematic review. Surg Infect. 2017;18:722-35. https://doi.org/10.1089/sur.2017.089
Davis SS, Husain FA, Lin E, Nandipati KC, Perez S, Sweeney JF. Resident participation in index laparoscopic general surgical cases: impact of the learning environment on surgical outcomes. J Am Coll Surg. 2013;216:96-104. https://doi.org/10.1016/j.jamcollsurg.2012.08.014
Paredes AZ, Hyer JM, Diaz A, Tsilimigras DI, Pawlik TM. The Impact of mental illness on postoperative outcomes among medicare beneficiaries: a missed opportunity to help surgical patients? Ann Surg. 2020;272:419-25. https://doi.org/10.1097/SLA.0000000000004118
Doering LV, Cross R, Vredevoe D, Martinez-Maza O, Cowan MJ. Infection, depression, and immunity in women after coronary artery bypass: a pilot study of cognitive behavioral therapy. Altern Ther Health Med. 2007;13:18-21.
Bozic KJ, Lau E, Kurtz S, Ong K, Berry DJ. Patient-related risk factors for postoperative mortality and peripros thetic joint infection in medicare patients undergoing TKA. Clin Orthop Relat Res. 2012;470:130-7. https://doi.org/10.1007/s11999-011-2043-3
Chang SM, Parney IF, McDermott M, Barker FG, Schmidt MH, Huang W, et al. Perioperative complications and neurological outcomes of first and second craniotomies among patients enrolled in the Glioma Outcome Project. J Neurosurg. 2003;98:1175-81. https://doi.org/10.3171/jns.2003.98.6.1175
Gordon RJ, Weinberg AD, Pagani FD, Slaughter MS, Pappas PS, Naka Y, et al. Prospective, multicenter study of ventricular assist device infections. Circulation. 2013;127:691-702. https://doi.org/10.1161/CIRCULATIONAHA.112.128132
Wang X, Zhang L, Lei Y, Liu X, Zhou X, Liu Y, et al. Meta-analysis of infectious agents and depression. Sci Rep. 2014;4:4530. https://doi.org/10.1038/srep04530
Kiecolt-Glaser JK, Glaser R. Depression and immune function: central pathways to morbidity and mortality. J Psychosom Res. 2002;53:873-6. https://doi.org/10.1016/S0022-3999(02)00309-4
Glaser R, Kiecolt-Glaser JK. Stress-induced immune dysfunction: implications for health. Nat Rev Immunol. 2005;5:243-51. https://doi.org/10.1038/nri1571
Irwin MR, Cole SW. Reciprocal regulation of the neural and innate immune systems. Nat Rev Immunol. 2011;11:625-32. https://doi.org/10.1038/nri3042
Sulzgruber P, Schnaubelt S, Koller L, Laufer G, Pilz A, Kazem N, et al. An extended duration of the pre-operative hospitalization is associated with an increased risk of healthcare-associated infections after cardiac surgery. Sci Rep. 2020;10:8006. https://doi.org/10.1038/s41598-020-65019-8
Leung Wai Sang S, Chaturvedi R, Alam A, Samoukovic G, de Varennes B, Lachapelle K. Preoperative hospital length of stay as a modifiable risk factor for mediastinitis after cardiac surgery. J Cardiothorac Surg. 2013;8:45. https://doi.org/10.1186/1749-8090-8-45
Montes FR, Vásquez SM, Camargo-Rojas CM, Rueda MV, Góez-Mogollón L, Alvarado PA, et al. Association between emergency department length of stay and adverse perioperative outcomes in emergency surgery: a cohort study in two Colombian University hospitals. BMC Emerg Med. 2019;19:27. https://doi.org/10.1186/s12873-019-0241-6
Stewart LM, Spangler EL, Sutzko DC, Pearce BJ, McFarland GE, Passman MA, et al. The association between preoperative length of stay and surgical site infection after lower extremity bypass for chronic limb-threatening ischemia. J Vasc Surg. 2021;73:1340-1349.e2. https://doi.org/10.1016/j.jvs.2020.08.037
Saban A, Shoham-Vardi I, Yohay D, Weintraub AY. Peritoneal adhesions are an independent risk factor for peri- and post-partum infectious morbidity. Eur J Obstet Gynecol Reprod Biol. 2019;241:60-5. https://doi.org/10.1016/j.ejogrb.2019.08.001
Van-Goor H. Consequences and complications of peritoneal adhesions. Colorectal Dis. 2007;9-Suppl2:25-34. https://doi.org/10.1111/j.1463-1318.2007.01358.x
Heniford BT, Ross SW, Wormer BA, Walters AL, Lincourt AE, Colavita PD, et al. Preperitoneal ventral hernia repair: a decade long prospective observational study with analysis of 1023 patient outcomes. Ann Surg. 2020;271:364-74. https://doi.org/10.1097/SLA.0000000000002966
Kao AM, Arnold MR, Augenstein VA, Heniford BT. Prevention and treatment strategies for mesh infection in abdominal wall reconstruction. Plast Reconstr Surg. 2018;142-Suppl3:149S-155S. https://doi.org/10.1097/PRS.0000000000004871
Hu T, Wu X, Hu J, Chen Y, Liu H, Zhou C, et al. Incidence and risk factors for incisional surgical site infection in patients with Crohn’s disease undergoing bowel resection. Gastroenterol Rep (Oxf). 2018;6:189-94. https://doi.org/10.1093/gastro/goy007
Kalakouti E, Simillis C, Pellino G, Mughal N, Warren O, Mills S, et al. Characteristics of surgical site infection following colorectal surgery in a tertiary center: extended-spectrum β-lactamase-producing bacteria culprits in disease. Wounds. 2017;30:108-13.
Kaoutzanis C, Leichtle SW, Mouawad NJ, Welch KB, Lampman RM, Wahl WL, et al. Risk factors for postoperative wound infections and prolonged hospitalization after ventral/incisional hernia repair. Hernia. 2015;19:113- 23. https://doi.org/10.1007/s10029-013-1155-y
Descargas
Publicado
Cómo citar
Número
Sección
Licencia
Derechos de autor 2022 Revista Colombiana de Cirugía

Esta obra está bajo una licencia internacional Creative Commons Atribución-NoComercial-SinDerivadas 4.0.
Todos los textos incluidos en la Revista Colombiana de Cirugía están protegidos por derechos de autor. Las opiniones expresadas en los artículos firmados son las de los autores y no coinciden necesariamente con las de los directores o los editores de la Revista Colombiana de Cirugía. Las sugerencias diagnósticas o terapéuticas como elección de productos, dosificación y métodos de empleo corresponden a la experiencia y al criterio de los autores.

















.jpg)


