Terapia endocrina para la prevención primaria del cáncer de seno: Revisión sistemática y metaanálisis actualizado
DOI:
https://doi.org/10.30944/20117582.1095Palabras clave:
metaanálisis, neoplasias de la mama, prevención & control, prevención primaria, moduladores selectivos de los receptores de estrógeno, inhibidores de la aromatasaResumen
Introducción. Debido a que el cáncer de seno es una enfermedad asociada a una significativa tasa de morbilidad y mortalidad cuando se diagnostica en el período sintomático, se han hecho enormes esfuerzos orientados hacia la prevención primaria de esta enfermedad.
Métodos. Se realizó una búsqueda de todos los experimentos clínicos aleatorizados que evaluaran la eficacia de la terapia endocrina para la reducción del riesgo de desarrollar cáncer de seno. La calidad metodológica de los estudios seleccionados fue valorada utilizando la herramienta de la Colaboración Cochrane para medir el riesgo de sesgo en ensayos aleatorizados. Se evaluó la heterogeneidad de los estudios primarios elegibles utilizando los estadísticos T², I², H². El sesgo de publicación fue evaluado mediante el test de Harbord y mediante la gráfica de funnel plot. La medida de efecto utilizada en este metaanálisis fue el riesgo relativo (RR) con el cálculo de los intervalos de confianza (IC) del 95%.
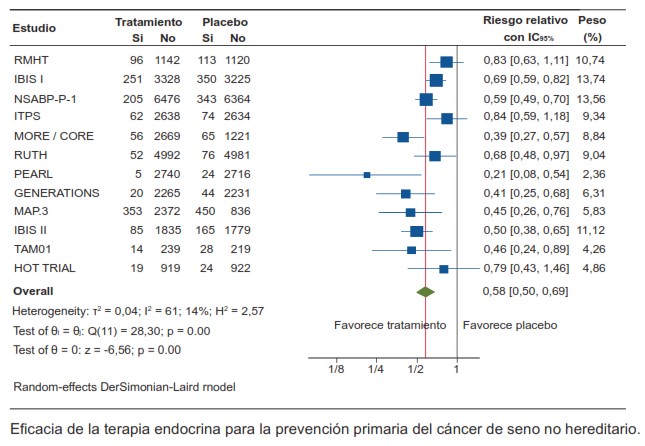
Resultados. Encontramos doce experimentos clínicos aleatorizados que reclutaron a 68.180 mujeres, las cuales fueron asignadas al azar para recibir algún tipo terapia endocrina para reducir el riesgo de desarrollar cáncer de seno o placebo. La terapia endocrina en conjunto redujo el riesgo proporcional de cáncer de seno (invasivo más in situ) en un 42 %, resultado estadísticamente significativo RR 0,58 (IC95% 0,50 – 0,69).
Conclusiones. La terapia endocrina es el manejo estándar de prevención en mujeres sanas con riesgo de desarrollar cáncer de seno no hereditario.
Descargas
Referencias bibliográficas
Toniolo PG, Levitz M, Zeleniuch-Jacquotte A, Banerjee S, Koenig KL, Shore RE, et al. A prospective study of endogenous estrogens and breast cancer in postmenopausal women. J Natl Cancer Inst. 1995;87:190-7. https://doi.org/10.1093/jnci/87.3.190
Santen RJ, Yue W, Naftolin F, Mor G, Berstein L. The potential of aromatase inhibitors in breast cancer prevention. Endocr Rel Cancer. 1999;6:235-43. https://doi.org/10.1677/erc.0.0060235
Simpson ER, Zhao Y, Agarwal VR, Michael MD, Bulun SE, Hinshelwood MM, et al. Aromatase expression in health and disease. Rec Prog Hormone Res. 1997;52:185–213.
Higgins J, Green S. Cochrane Handbook for Systematic Reviews of Interventions Version 5.1.0. The Cochrane Collaboration; 2011. Disponible en: https://www.cochranehandbook.org/
Tricco AC, Tetzlaff J, Moher D. The art and science of knowledge synthesis. J Clin Epidemiol. 2011;64:11-20. https://doi.org/10.1016/j.jclinepi.2009.11.007
Higgins JPT, Altman DG, Gøtzsche PC, Jüni P, Moher D, Oxman AD, et al. The Cochrane Collaboration’s tool for assessing risk of bias in randomized trials. BMJ. 2011;343:d5928. https://doi.org/10.1136/bmj.d5928
Higgins JPT, Thompson SG. Quantifying heterogeneity in a meta-analysis. Stats Med. 2002;21:1539-58. https://doi.org/10.1002/sim.1186
Galbraith RF. Graphical display of estimates having differing standard errors. Technometrics. 1998;30:271- 81. https://doi.org/10.2307/1270081
L’Abbé KA, Detsky AS, O’Rourke K. Meta-analysis in clinical research. Ann Intern Med. 1987;107:224-33. https://doi.org/10.7326/0003-4819-107-2-224
Harbord RM, Egger M, Sterne JAC. Modified test for small-study efects in meta-analyses of controlled trials with binary endpoints. Statist Med. 2006;25:3443-57. https://doi.org/10.1002/sim.2380
Sterne JAC, Egger M. Funnel plots for detecting bias in meta-analysis: Guidelines on choice of axis. J Clin Epidemiol. 2001;54:1046-55. https://doi.org/10.1016/s0895-4356(01)00377-8
Bolaños-Díaz R, Calderón-Cahua M. Introducción al meta-análisis tradicional. Rev Gastroenterol Peru. 2014;34:45-51.
Page MJ, McKenzie JE, Bossuyt PM, Hoffmann TC, Mulrow CD, Shamseer L, et al. The PRISMA 2020 statement: an updated guideline for reporting systematic reviews. BMJ. 2021;372:n71. https://doi.org/10.1136/bmj.n71
Cuzick J, Powles T, Veronesi U, Forbes J, Edwards R, Ashley S, Boyle P. Overview of the main outcomes in breast-cancer prevention trials. Lancet. 2003;361:296- 300. https://doi.org/10.1016/S0140-6736(03)12342-2
Cuzick J, Sestak I, Bonanni B, Costantino JP, Cummings S, DeCensi A, et al. Selective oestrogen receptor modulators in prevention of breast cancer: an updated meta-analysis of individual participant data. Lancet. 2013;381:1827-34. https://doi.org/10.1016/S0140-6736(13)60140-3
Mocellin S, Pilati P, Briarava M, Nitti D. Breast cancer chemoprevention: A network meta-analysis of randomized controlled trials. J Natl Cancer Inst. 2016;108:1- 9. https://doi.org/10.1093/jnci/djv318
Mocellin S, Goodwin A, Pasquali S. Risk-reducing medications for primary breast cancer: a network meta-analysis. Cochrane Database Syst Rev. 2019;4:CD012191. https://doi.org/10.1002/14651858.CD012191.pub2
Vogel VG, Costantino JP, Wickerham DL, Cronin WM, Cecchini RS, Atkins JN, et al. Effects of tamoxifen vs raloxifene on the risk of developing invasive breast cancer and other disease outcomes: the NSABP Study of Tamoxifen and Raloxifene (STAR) P-2 Trial. JAMA. 2006;295:2727–41. https://doi.org/10.1001/jama.295.23.joc60074
Vogel VG, Costantino JP, Wickerham DL, Cronin WM, Cecchini RS, Atkins JN, et al. Update of the National Surgical Adjuvant Breast and Bowel Project Study of Tamoxifen and Raloxifene (STAR) P-2 Trial: preventing breast cancer. Cancer Prev Res. 2010;3:696-706. https://doi.org/10.1158/1940-6207.CAPR-10-0076
Decensi A, Robertson C, Guerrieri-Gonzaga A, Serrano D, Cazzaniga M, Mora S, et al. Randomized doubleblind 2 x 2 trial of low-dose tamoxifen and fenretinide for breast cancer prevention in high-risk premenopausal women. J Clin Oncol. 2009;27:3749-56. https://doi.org/10.1200/JCO.2008.19.3797
Cummings SR, Black DM, Thompson DE, Applegate WB, Barrett-Connor E, Musliner TA, et al. Effect of alendronate on risk of fracture in women with low bone density but without vertebral fractures: results from the Fracture Intervention Trial. JAMA. 1998;280:2077-82. https://doi.org/10.1001/jama.280.24.2077
Black DM, Delmas PD, Eastell R, Reid IR, Boonen S, Cauley JA, et al. Once-yearly zoledronic acid for treatment of postmenopausal osteoporosis. N Engl J Med. 2007;356:1809-22. https://doi.org/10.1056/NEJMoa067312
Cummings SR, Ettinger B, Delmas PD, Kenemans P, Stathopoulos V, Verweij P, et al. The effects of tibolone in older postmenopausal women. N Engl J Med. 2008;359:697-708. https://doi.org/10.1056/NEJMoa0800743
Cook NR, Lee IM, Zhang SM, Moorthy MV, Buring JE. Alternate-day, low-dose aspirin and cancer risk: long-term observational follow-up of a randomized trial. Ann Intern Med. 2013;159:77-85. https://doi. org/10.7326/0003-4819-159-2-201307160-00002
Rothwell PM, Price JF, Fowkes FG, Zanchetti A, Roncaglioni MC, Tognoni G, et al. Short-term effects of daily aspirin on cancer incidence, mortality, and non-vascular death: analysis of the time course of risks and benefits in 51 randomised controlled trials. Lancet. 2012;379:1602-12. https://doi.org/10.1016/S0140-6736(11)61720-0
Lee IM, Cook NR, Manson JE, Buring JE, Hennekens CH. Beta-carotene supplementation and incidence of cancer and cardiovascular disease: the Women’s Health Study. J Natl Cancer Inst. 1999;91:2102-6. https://doi.org/10.1093/jnci/91.24.2102
Hercberg S, Galan P, Preziosi P, Bertrais S, Mennen L, Malvy D, et al. The SU.VI.MAX Study: a randomized, placebo-controlled trial of the health effects of antioxidant vitamins and minerals. Arch Intern Med. 2004;164:2335-42. https://doi.org/10.1001/archinte.164.21.2335
Avenell A, MacLennan GS, Jenkinson DJ, McPherson GC, McDonald AM, Pant PR, et al. Long-term follow-up for mortality and cancer in a randomized placebo-controlled trial of vitamin D(3) and/or calcium (RECORD trial). J Clin Endocrinol Metab. 2012;97:614-22. https://doi.org/10.1210/jc.2011-1309
Lappe JM, Travers-Gustafson D, Davies KM, Recker RR, Heaney RP. Vitamin D and calcium supplementation reduces cancer risk: results of a randomized trial. Am J Clin Nutr. 2007;85:1586-91. https://doi.org/10.1093/ajcn/85.6.1586
Chlebowski RT, Johnson KC, Kooperberg C, Pettinger M, Wactawski-Wende J, Rohan T, et al. Calcium plus vitamin D supplementation and the risk of breast cancer. J Natl Cancer Inst. 2008;100:1581-91. https://doi.org/10.1093/jnci/djn360
Trivedi DP, Doll R, Khaw KT. Effect of four monthly oral vitamin D3 (cholecalciferol) supplementation on fractures and mortality in men and women living in the community: randomised double blind controlled trial. BMJ. 2003;326:469. https://doi.org/10.1136/bmj.326.7387.469
Lee IM, Cook NR, Gaziano JM, Gordon D, Ridker PM, Manson JE, et al. Vitamin E in the primary prevention of cardiovascular disease and cancer: the Women’s Health Study: a randomized controlled trial. JAMA. 2005;294:56-65. https://doi.org/10.1001/jama.294.1.56
Vollset SE, Clarke R, Lewington S, Ebbing M, Halsey J, Lonn E, et al. Effects of folic acid supplementation on overall and site-specific cancer incidence during the randomised trials: meta-analyses of data on 50,000 individuals. Lancet. 2013;381:1029-36. https://doi.org/10.1016/S0140-6736(12)62001-7
Downs JR, Clearfield M, Weis S, Whitney E, Shapiro DR, Beere PA, et al. Primary prevention of acute coronary events with lovastatin in men and women with average cholesterol levels: results of AFCAPS/TexCAPS. Air Force/Texas Coronary Atherosclerosis Prevention Study. JAMA. 1998;279:1615-22. https://doi.org/10.1001/jama.279.20.1615
Sacks FM, Pfeffer MA, Moye LA, Rouleau JL, Rutherford JD, Cole TG, et al. The effect of pravastatin on coronary events after myocardial infarction in patients with average cholesterol levels. Cholesterol and Recurrent Events Trial investigators. N Engl J Med. 1996;335:1001-9. https://doi.org/10.1056/NEJM199610033351401
The Long-Term Intervention with Pravastatin in Ischaemic Disease (LIPID) Study Group. Prevention of cardiovascular events and death with pravastatin in patients with coronary heart disease and a broad range of initial cholesterol levels. N Engl J Med. 1998;339:1349-57. https://doi.org/10.1056/NEJM199811053391902
ALLHAT Officers and Coordinators for the ALLHAT Collaborative Research Group. Major outcomes in moderately hypercholesterolemic, hypertensive patients randomized to pravastatin vs usual care: The Antihypertensive and Lipid-Lowering Treatment to Prevent Heart Attack Trial (ALLHAT-LLT). JAMA. 2002;288:2998-3007. https://doi.org/10.1001/jama.288.23.2998
Shepherd J, Blauw GJ, Murphy MB, Bollen EL, Buckley BM, Cobbe SM, et al. Pravastatin in elderly individuals at risk of vascular disease (PROSPER): a randomised controlled trial. Lancet. 2002;360:1623-30. https://doi.org/10.1016/s0140-6736(02)11600-x
Heart Protection Study Collaborative Group. MRC/BHF Heart Protection Study of cholesterol lowering with simvastatin in 20,536 high-risk individuals: a randomised placebo-controlled trial. Lancet. 2002;360:7-22. https://doi.org/10.1016/S0140-6736(02)09327-3
Strandberg TE, Pyörälä K, Cook TJ, Wilhelmsen L, Faergeman O, Thorgeirsson G, et al. Mortality and incidence of cancer during 10-year follow-up of the Scandinavian Simvastatin Survival Study (4S). Lancet. 2004;364:771- 7. https://doi.org/10.1016/S0140-6736(04)16936-5
Forbes JF, Sestak I, Howell A, Bonanni B, Bundred N, Levy C, et al. Anastrozole versus tamoxifen for the prevention of locoregional and contralateral breast cancer in postmenopausal women with locally excised ductal carcinoma in situ (IBIS-II DCIS): a double blind, randomised controlled trial. Lancet. 2016;387:866-73. https://doi.org/10.1016/S0140-6736(15)01129-0
Powles TJ, Ashley S, Tidy A, Smith IE, Dowsett M. Twenty-year follow-up of the Royal Marsden randomized, double-blinded tamoxifen breast cancer prevention trial. J Natl Cancer Inst. 2007;99:283-90. https://doi.org/10.1093/jnci/djk050
Cuzick J, Sestak I, Cawthorn S, Hamed H, Holli K, Howell A, et al. Tamoxifen for prevention of breast cancer: extended long-term follow-up of the IBIS-I cancer prevention trial. Lancet Oncol. 2015;16:67-75. https://doi.org/10.1016/S1470-2045(14)71171-4
Fisher B, Costantino JP, Wickerham DL, Cecchini RS, Cronin WM, Robidoux A, et al. Tamoxifen for the prevention of breast cancer: current status of the National Surgical Adjuvant Breast and Bowel Project P-1 study. J Natl Cancer Inst. 2005;97:1652-62. https://doi.org/10.1093/jnci/dji372
Veronesi U, Maisonneuve P, Rotmensz N, Bonanni B, Boyle P, Viale G, et al. Tamoxifen for the prevention of breast cancer: Late results of the Italian Randomized Tamoxifen Prevention Trial among women with hysterectomy. J Natl Cancer Inst. 2007;99:727-37. https://doi.org/10.1093/jnci/djk154
Martino S, Cauley JA, Barrett-Connor E, Powles TJ, Mershon J, Disch D, et al. Continuing outcomes relevant to Evista: breast cancer incidence in postmenopausal osteoporotic women in a randomized trial of raloxifene. J Natl Cancer Inst. 2004;96:1751-61. https://doi.org/10.1093/jnci/djh319
Descargas
Publicado
Cómo citar
Número
Sección
Licencia
Derechos de autor 2022 Revista Colombiana de Cirugía

Esta obra está bajo una licencia internacional Creative Commons Atribución-NoComercial-SinDerivadas 4.0.
Todos los textos incluidos en la Revista Colombiana de Cirugía están protegidos por derechos de autor. Las opiniones expresadas en los artículos firmados son las de los autores y no coinciden necesariamente con las de los directores o los editores de la Revista Colombiana de Cirugía. Las sugerencias diagnósticas o terapéuticas como elección de productos, dosificación y métodos de empleo corresponden a la experiencia y al criterio de los autores.

















.jpg)


